Transcranial Magnetic Stimulation (TMS) is no longer considered a “last resort” treatment. Many psychiatrists and clinics now integrate it earlier in the care process for patients struggling with depression, anxiety, or other treatment-resistant mental health conditions. If you’re a provider, recognizing when to refer a patient for TMS can help improve outcomes, reduce symptom duration, and minimize the risks associated with prolonged medication trials. Below, we’ll cover three clear signs that it may be time to make that referral—and how identifying them early can make a significant difference in patient recovery. Understanding TMS in the Treatment Landscape TMS is an FDA-cleared, non-invasive treatment that uses magnetic pulses to stimulate areas of the brain linked to mood regulation. It’s generally well-tolerated, requires no anesthesia, and allows patients to resume daily activities immediately after each session. For patients who haven’t responded to traditional interventions, TMS offers a path forward without many of the side effects associated with medications or the invasiveness of other procedures. Referring a patient for TMS is not about “giving up” on other treatments—it’s about offering the right tool at the right time in their care plan. Sign 1: Limited Response to Antidepressants or Medication Intolerance One of the most common reasons to refer a patient for TMS is a lack of meaningful improvement after trying one or more antidepressants. If a patient has undergone multiple medication trials without achieving remission, TMS can provide a new pathway forward. In some cases, patients do respond to medication but cannot tolerate the side effects—such as weight gain, sexual dysfunction, sedation, or gastrointestinal issues. This leads to poor adherence and, ultimately, relapse. TMS avoids systemic side effects because it works locally on the brain rather than circulating through the body. Quick checklist for providers: Sign 2: Early Signs of Treatment Resistance Treatment-resistant depression (TRD) doesn’t happen overnight—it develops over time when patients consistently fail to achieve relief from standard interventions. Early identification of treatment resistance can shorten the time to remission and prevent unnecessary suffering. If a patient is showing early warning signs—such as persistent depressive episodes despite medication adjustments—it may be appropriate to refer a patient for TMS before symptoms become entrenched. Why timing matters: Sign 3: Preference for Non-Pharmacological or Non-Invasive Options Some patients are hesitant to start or continue psychiatric medications due to personal preference, past experiences, or medical contraindications. Others may want a treatment option that fits seamlessly into their daily lives without downtime or recovery. In these situations, TMS is often an ideal match. It’s conducted in an outpatient setting, typically takes about 20 minutes per session, and allows patients to drive themselves to and from appointments. When to consider referral: Why Proactive Referrals Matter Waiting until all other options are exhausted can prolong patient suffering and make recovery more difficult. As evidence for TMS continues to grow, proactive referrals are becoming the standard among forward-thinking psychiatric providers. By knowing when to refer a patient for TMS, you can help patients access a proven, safe, and effective treatment sooner. The Takeaway on When to Refer a Patient for TMS If your patient is showing signs of medication failure, developing treatment resistance, or seeking a non-invasive option, TMS may be the next step. Early referral can improve response rates, preserve quality of life, and give patients hope when other treatments have fallen short. Learn more about the Blossom TMS Therapy System and how it can fit into your practice to better serve your patients.Blossom TMS Therapy SystemPhone: 833.3BUY.TMS (+1.833.3289.867)Email: Sales@sebersmedical.comAddress: 230 S Broad Street, 17th Floor Philadelphia, PA 19102
Understanding the Real Differences in TMS vs ECT
If you’ve been exploring treatment options for depression, anxiety, or other mental health conditions, you may have come across two terms: TMS and ECT. While both are brain-based treatments, comparing them directly can lead to confusion—and sometimes fear. Let’s clear it up. At SEBERS Medical, we believe in offering innovative solutions grounded in science, safety, and comfort. Here are 3 key reasons why the TMS vs ECT comparison isn’t apples to apples—and why Transcranial Magnetic Stimulation (TMS) stands in a category of its own. 1. TMS vs ECT: No Anesthesia, No Downtime One of the most important distinctions in the TMS vs ECT conversation is how the procedures are performed. Electroconvulsive therapy (ECT) requires general anesthesia because the treatment intentionally induces a seizure. This process means patients must fast beforehand, be monitored post-procedure, and often need a ride home. TMS, on the other hand, is non-invasive and does not require any anesthesia. You remain fully awake and alert during the session, which typically lasts about 20 minutes. Most patients describe the sensation as a gentle tapping on the scalp. After your TMS session, you can immediately return to: No grogginess. No recovery room. No need for a chaperone. Just walk in, receive your treatment, and walk out. 2. TMS vs ECT: No Seizures, No Systemic Shock It’s important to understand that ECT involves controlled seizure induction. While effective for some patients with treatment-resistant depression, this process can lead to temporary confusion, memory issues, and other cognitive side effects. TMS is entirely different. It uses magnetic pulses to gently stimulate specific regions of the brain, particularly the prefrontal cortex, which is often underactive in individuals with depression. This stimulation promotes new neural activity without causing a seizure. Key differences in side effects: Side Effect ECT TMS Memory Loss Common Rare Anesthesia Risks Yes No Confusion/Disorientation Often Rare Headache or Scalp Discomfort Occasionally Occasionally In the TMS vs ECT conversation, this is where TMS often wins people over—it delivers targeted treatment without the systemic shock. 3. TMS vs ECT: Fewer Side Effects, Greater Accessibility ECT has long been a last-resort treatment for severe, unresponsive depression. But its intensity, required hospital visits, and potential cognitive effects make it less accessible or appealing for many patients. TMS, however, is increasingly becoming a first-line treatment for individuals who haven’t found relief through medication or talk therapy. It’s FDA-cleared, backed by growing clinical evidence, and covered by most insurance providers. Patients typically undergo TMS five days a week for 4–6 weeks. Because there’s no anesthesia involved and side effects are minimal, TMS is far more accessible for working professionals, students, and busy parents. In summary, here’s why more psychiatrists and patients are turning to TMS: What Patients Are Saying “I was hesitant when I heard ‘brain stimulation,’ but the staff walked me through the process, and it couldn’t have been easier. I was in and out and felt like myself again after a few weeks.” “My medications weren’t helping, and I didn’t want to try ECT. TMS was the best decision I’ve made.” Final Thoughts: Choosing the Right Path While TMS and ECT both aim to relieve symptoms of severe mental illness, they are vastly different in method, side effects, and patient experience. For individuals seeking a less invasive, more lifestyle-friendly treatment, TMS is a promising solution. Still unsure whether TMS is right for you or your clinic? SEBERS Medical is here to help. Explore more about Transcranial Magnetic Stimulation and see how SEBERS Medical supports clinicians and providers’ TMS technology.Visit https://blossomtms.com Address: 230 S Broad Street, 17th Floor, Philadelphia, PA 19102Phone: 833.3BUY.TMS (+1.833.3289.867) Email: Sales@sebersmedical.com
The Expanding Role of TMS in Modern Psychiatry
Transcranial Magnetic Stimulation (TMS) is not just an emerging tool—it is a central figure in the evolving landscape of mental health treatment. As research continues to uncover its efficacy across multiple psychiatric conditions, the time is ripe to re-evaluate the role of TMS in modern psychiatry. While traditionally considered a last-resort treatment for major depressive disorder, TMS is steadily gaining traction as a first-line or adjunct option for a variety of hard-to-treat conditions. From bipolar depression to anxiety and PTSD, clinical data is reinforcing what many clinicians already observe in practice: TMS offers reliable relief without the burdens of medication side effects or invasive procedures. Why Reassess TMS in Modern Psychiatry? The psychiatric field is at a pivotal moment. Medications remain foundational, but they don’t work for everyone. Roughly one-third of patients with major depressive disorder are treatment-resistant, and similar challenges exist for bipolar disorder and anxiety. That’s where TMS in modern psychiatry starts to shine—offering both safety and adaptability in treatment-resistant populations. Here are some compelling areas where TMS is reshaping outcomes: Bipolar Depression: Encouraging Data for a Complex Diagnosis Managing bipolar depression is one of the most difficult tasks in psychiatry. Antidepressants can risk mood destabilization, and many patients cycle through ineffective regimens. TMS presents a compelling, non-pharmacological alternative. A systematic review of 12 clinical studies analyzing TMS outcomes in bipolar depression revealed moderate-to-large improvements in depressive symptoms, particularly among treatment-resistant individuals. Response rates reached approximately 54%, and remission rates were similarly promising. Key findings from the review include: This evidence supports a broader and earlier use of TMS in modern psychiatry, particularly for patients struggling with mood instability and medication fatigue. Anxiety: Quieting the Nervous System The role of TMS in modern psychiatry extends well beyond depression. Generalized anxiety disorder (GAD), panic disorder, and social anxiety often coexist with mood disorders, complicating treatment plans. A meta-analysis of 10 studies found that TMS, particularly when targeting the right dorsolateral prefrontal cortex (rDLPFC), led to moderate reductions in anxiety symptoms across multiple diagnoses. Given the non-systemic nature of TMS, it’s an ideal choice for patients who experience poor tolerance to benzodiazepines or SSRIs. Furthermore, the rise of personalized protocols has made TMS even more viable. Clinicians are now using EEG-informed coil placement and adjusting stimulation frequency to match individual brain profiles—creating a more targeted approach to anxiety relief. PTSD and Beyond: A Window Into Neural Reset Post-traumatic stress disorder (PTSD) is another condition where TMS in modern psychiatry is showing significant promise. Randomized clinical trials in veterans and civilians report meaningful reductions in symptoms, particularly when TMS is integrated with trauma-informed psychotherapy. The mechanism is thought to involve rebalancing activity in brain regions tied to emotion regulation, such as the amygdala and medial prefrontal cortex. This effect can improve emotional processing, reduce reactivity, and support long-term healing—all without pharmacological intervention. Personalized Psychiatry: The Real Promise of TMS What makes TMS in modern psychiatry truly exciting is its flexibility. With customizable frequencies (1 Hz, 10 Hz, theta burst), session durations, and coil types (figure-8, H-coils), psychiatrists now have an adaptable tool that can meet the unique neural signatures of each patient. Emerging innovations in neuronavigation and quantitative EEG mapping make targeting even more precise, allowing clinicians to identify underactive or overactive brain regions with increasing accuracy. “The future of psychiatry lies in personalization—and TMS is already there. It’s the first tool I reach for when medication has failed or isn’t an option.”— Dr. L. Kumar, Board-Certified Psychiatrist This level of precision doesn’t just improve outcomes—it strengthens the therapeutic alliance. Patients feel that their treatment is tailored to their needs, and providers have objective data to guide decision-making. Fewer Side Effects, More Patient Adherence Another major advantage of TMS is its minimal side-effect profile. Unlike antidepressants or mood stabilizers, TMS does not cause weight gain, sexual dysfunction, sedation, or cognitive dulling. For many patients, this leads to higher treatment adherence and greater satisfaction. Additionally, recent developments such as intermittent theta burst stimulation allow for shorter treatment sessions, sometimes as brief as three minutes. This convenience allows patients to fit TMS into their daily lives without disruption—an important consideration for working professionals, caregivers, and students. A Call to Action for Providers and Clinics As the evidence base grows, it’s clear that TMS in modern psychiatry deserves more than niche status. Psychiatrists, therapists, and healthcare systems should consider expanding access to TMS not just as a fallback, but as a proactive treatment strategy. Whether integrated into outpatient clinics, hospitals, or private practice, TMS represents an opportunity to elevate standards of care and offer hope to individuals who have long struggled to find relief. Devices like the Blossom TMS are designed to meet that demand—providing reliable performance, precision targeting, and support for a wide range of treatment protocols. The Future of Psychiatry is Magnetic The conversation around TMS in modern psychiatry is changing—and for good reason. With strong clinical data, minimal side effects, and unmatched flexibility, TMS is more than a treatment; it’s a paradigm shift. Whether used for bipolar depression, anxiety, PTSD, or treatment-resistant unipolar depression, it offers a patient-centric, evidence-based solution with room for innovation. Now is the time to embrace the full potential of this transformative tool. Learn more about Blossom TMS and explore how TMS can fit into your practice.Visit https://blossomtms.comPhone: 833.3BUY.TMS (833.3289.867)Email: Sales@sebersmedical.comAddress: 230 S Broad Street, 17th Floor, Philadelphia, PA 19102
Why Your Antidepressant Might Not Be Enough: Understanding Treatment-Resistant Depression
For millions of people living with depression, finding relief isn’t as simple as taking a single pill. Many patients try one, two, even three medications without seeing meaningful change. This frustrating cycle is more than just bad luck—it may be a sign of treatment-resistant depression, a condition that requires a different kind of support. What Is Treatment-Resistant Depression? Treatment-resistant depression (TRD) is diagnosed when a person with major depressive disorder doesn’t respond to at least two different antidepressant medications, each taken at an appropriate dose and duration. If you’ve been through several rounds of medications with little to no improvement, you may be dealing with TRD—and you’re not alone. According to research, up to one-third of patients with depression don’t find adequate relief from traditional antidepressants. It’s not a reflection of willpower, motivation, or effort. Rather, it suggests that your brain may need a more targeted intervention—one that goes beyond chemistry alone. Why Antidepressants Aren’t Always Enough Antidepressants work by shifting levels of neurotransmitters like serotonin, dopamine, or norepinephrine. However, their effects are systemic, meaning they impact the entire body—not just the parts of the brain responsible for mood. That’s why some people experience side effects like weight changes, sexual dysfunction, insomnia, or emotional blunting. In cases of treatment-resistant depression, the issue may lie in the brain’s electrical activity rather than chemical imbalances alone. If medications haven’t reached the source of your symptoms, no dosage adjustment will fully address the problem. That’s where Transcranial Magnetic Stimulation (TMS) comes in. How TMS Treats Treatment-Resistant Depression Differently TMS is a non-invasive, FDA-cleared treatment for treatment-resistant depression that stimulates the brain directly using magnetic pulses. Instead of affecting the whole body like medication, TMS zeroes in on the prefrontal cortex—a key region involved in emotional regulation and decision-making. Key Benefits of TMS for Treatment-Resistant Depression Over the course of 4 to 6 weeks, patients undergo regular TMS sessions, gradually restoring healthier brain activity patterns associated with mood improvement and emotional clarity. Is TMS Right for You? If you or someone you love has been struggling with treatment-resistant depression, you may feel like you’ve exhausted every option. TMS offers new hope, especially for those who: At SEBERS Medical, we’re proud to distribute the most advanced, research-backed TMS systems available today. We partner with clinics, providers, and practices across the country who want to bring high-quality TMS care to their communities. Reclaim Control Over Your Mental Health Depression doesn’t always respond to the first treatment—or even the second. That doesn’t mean recovery is out of reach. With the right tools, including innovative therapies like TMS, relief from treatment-resistant depression is possible. We believe in solutions that go beyond symptom management. Whether you’re a patient looking for answers or a clinic ready to expand your mental health services, SEBERS Medical is here to help you take the next step forward. Learn more about our TMS technology and find out how Blossom TMS can support individuals facing treatment-resistant depression by visiting: SEBERS Medical 230 S Broad Street, 17th Floor, Philadelphia, PA 19102 Phone: 833.3BUY.TMS (+1.833.3289.867) Email: Sales@sebersmedical.com
How TMS Targets the DLPFC—And Why That Matters
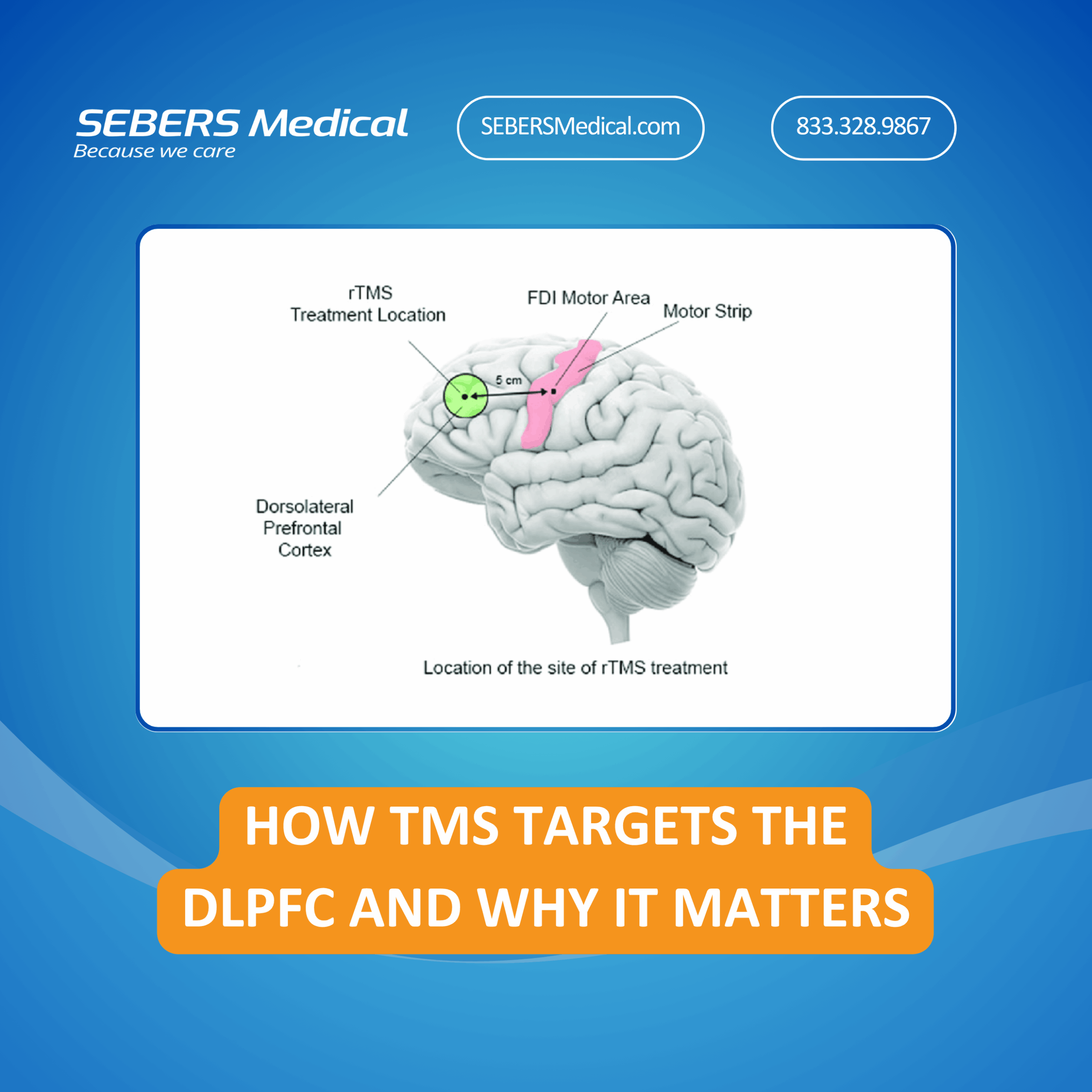
Transcranial Magnetic Stimulation (TMS) is more than just a buzzword in modern psychiatry—it’s a scientifically backed, FDA-cleared treatment that offers new hope for people with treatment-resistant depression. But while the therapy itself may seem cutting-edge, understanding why it works can bring powerful insight to both patients and providers. One of the most vital components of TMS therapy is its precision: TMS targets the DLPFC (dorsolateral prefrontal cortex), a key region in the brain associated with mood regulation, cognitive control, and emotional resilience. So what exactly is the DLPFC—and why is it the focus of TMS? Let’s break it down. What Is the DLPFC? The dorsolateral prefrontal cortex (DLPFC) is a region in the frontal lobe of the brain. It’s responsible for higher-level executive functions such as decision-making, problem-solving, planning, emotional regulation, and working memory. In simple terms, the DLPFC helps you stay focused, balanced, and emotionally engaged with the world around you. In individuals with depression, the DLPFC often becomes underactive, meaning it isn’t firing as it should. This leads to symptoms like low mood, impaired motivation, reduced concentration, and a general sense of emotional blunting or detachment. That’s where TMS comes in. Why TMS Targets the DLPFC TMS (Transcranial Magnetic Stimulation) uses highly focused magnetic pulses to stimulate nerve cells in the brain. These pulses are delivered non-invasively through a treatment coil placed over the scalp, with precision targeting of the left DLPFC, a region shown to be hypoactive in depression. TMS targets the DLPFC because activating this area helps restore functional connectivity and neurotransmitter activity that support healthy emotional processing. In clinical studies, patients who respond to TMS show increased metabolic activity in the DLPFC and improved communication between brain networks involved in mood regulation. This is not random stimulation—it’s targeted therapy guided by neuroimaging, research, and decades of neuroscience. Clinical Significance: The DLPFC and Depression Understanding why TMS targets the DLPFC gives deeper insight into how depression affects the brain. Studies using PET and fMRI scans have repeatedly shown that the DLPFC is less active in patients with major depressive disorder (MDD). This underactivity disrupts communication between other parts of the brain, including the limbic system (which governs emotion) and the anterior cingulate cortex (which helps monitor conflict and behavior). In effect, the DLPFC acts like a control hub for the emotional brain. When it’s not functioning properly, negative thought patterns, emotional numbness, and lack of motivation can dominate a person’s experience. By targeting and stimulating this area with magnetic pulses, TMS can effectively “wake up” this hub—leading to improvements in mood, clarity, and even energy levels. TMS: Precision with Purpose TMS is not a one-size-fits-all therapy. Treatment protocols are carefully mapped to deliver stimulation specifically to the left DLPFC, typically 5 days a week over 4 to 6 weeks. Some advanced systems use MRI-guided targeting or proprietary mapping algorithms to further enhance accuracy and patient outcomes. Because TMS targets the DLPFC directly, the treatment bypasses the gastrointestinal and systemic side effects that often accompany antidepressant medications. There’s no need for sedation or recovery time, and most patients return to their normal activities immediately after each session. For many, this targeted and non-invasive approach is the breakthrough they’ve been waiting for—especially after trying multiple medications with limited success. The Future of Targeted Mental Health Care We believe that informed treatment is powerful treatment. Understanding where and why TMS works helps clinicians refine care plans and empowers patients to take control of their mental health. By acknowledging that depression is a neurobiological condition with real structural and functional changes in the brain, we can move away from trial-and-error approaches and toward interventions grounded in science. TMS targets the DLPFC because that’s where depression often lives—and where healing can begin. Learn More or Get Started SEBERS Medical is committed to supporting providers and clinics with the highest quality in TMS technology, training, and resources. Whether you’re exploring new solutions for your patients or expanding your practice’s interventional psychiatry offerings, we’re here to help. Visit BlossomTMS.com to learn more about our state-of-the-art TMS systems. Phone: 833.3BUY.TMS (+1.833.3289.867)Email: Sales@sebersmedical.comAddress: 230 S Broad Street, 17th Floor, Philadelphia, PA 19102
Blossom TMS Provider Spotlight: Meet Our CEO, Christian Hirschbeck
Welcome to another edition of the Blossom TMS Provider Spotlight series, where we showcase key figures making waves in the TMS industry. Today, we’re excited to sit down with Christian Hirschbeck, our very own CEO at SEBERS Medical. Christian has over 15 years of experience in the field of TMS and neurostimulation, leading the way with innovative solutions like the Blossom TMS device. Let’s get to know him better and dive into his journey with TMS, his vision for the future, and the work he’s doing at SEBERS Medical. Blossom TMS: Christian, thank you for joining us! Can you tell us how you first got involved with TMS? Christian Hirschbeck:It’s great to be here! My journey with TMS started over 15 years ago when I was working for a neurophysiology company. We had a joint venture with a TMS startup, and that’s where I had my first contact with the technology. I was managing parts of product development for EEG solutions at the time, and we began exploring the combination of EEG and EMG with TMS. We were part of the manufacturing of the first German-made TMS stimulator on the market, and from there, we helped establish TMS in Germany. Blossom TMS: What drew you to TMS as a field?Christian Hirschbeck:What attracted me to TMS was its potential to not only diagnose but also treat patients. In neurophysiology, most of the focus is on diagnosis, but TMS opened up the possibility of actually helping patients improve their quality of life. That was a major factor for me. Being able to not only identify problems but provide a solution really stood out. Blossom TMS: What is your technical background, and how did that play a role in developing TMS technology? Christian Hirschbeck:I’m an electrical engineer by training, originally from Austria. My early career was in telecommunications, but I transitioned to neurostimulation and eventually became focused on sales and marketing. My technical background helps me understand the mechanics behind TMS devices, which has been invaluable as we’ve developed the Blossom TMS machine. While today’s devices are much more advanced than the older models, that engineering knowledge is still a huge advantage. Blossom TMS: How did the Blossom TMS device come about?Christian Hirschbeck:The Blossom TMS device was born out of a desire to make TMS more accessible and easier to use in clinical settings. Many devices on the market are research-focused, with too many complicated controls. We wanted to create a streamlined, easy-to-use device that could be widely adopted by clinicians. That’s where our slogan, “We Make TMS Easy,” comes from. I firmly believe that simplicity is the key to making TMS a go-to treatment. Blossom TMS: What makes the Blossom TMS device stand out from others on the market? Christian Hirschbeck:One of the biggest differentiators is our coil cooling system. We partnered with a Korean company, REMED, to ensure that we had the most reliable coil cooling on the market. Oil cooling, in particular, is key for performance and longevity, allowing our machines to run all day without overheating. Most devices use air cooling, which doesn’t perform as well, especially in warmer climates. Our oil-based cooling system ensures that the Blossom TMS is reliable, low maintenance, and incredibly efficient. Blossom TMS: What’s your vision for the future of TMS? Christian Hirschbeck:I see TMS evolving beyond just mental health treatments. While depression treatment is currently the most common use, I believe that TMS has huge potential in neurology, particularly in areas like stroke rehabilitation and pain management. In the future, I think TMS could become a standard tool in hospitals worldwide, just like EEG and EMG devices. At SEBERS Medical, we’re already working on expanding TMS applications to include neurology. Blossom TMS: You’ve worked hard to make the Blossom TMS device affordable. Why is that important to you? Christian Hirschbeck:Affordability is crucial if we want to see TMS become more widely used. At SEBERS Medical, we’re a privately owned company, so we don’t have investors pressuring us to inflate prices. We can focus on creating high-quality devices at reasonable prices. I don’t think that machines costing over $100,000 are the future of TMS. Devices like the Blossom TMS, which are priced around $50,000, will help make TMS more accessible to clinicians and, in turn, more available to patients.Blossom TMS: What challenges do new TMS providers face, and how does SEBERS Medical help? Christian Hirschbeck:New providers face two main challenges: technical concerns and business operations. On the technical side, we ensure that our machines are low-maintenance with no hidden fees like pay-per-use charges. On the business side, we offer extensive support, from training on how to use the machines to guidance on coding, insurance reimbursement, and even marketing. Our goal is to make the transition into offering TMS as seamless as possible for clinics. Blossom TMS: Finally, what’s next for SEBERS Medical and the Blossom TMS device? Christian Hirschbeck:We’re constantly looking for ways to innovate and improve. We’re working on expanding the clinical applications of TMS while maintaining the affordability and ease of use that we’ve become known for. We believe that the future of TMS is bright, and we’re excited to be part of that journey. At SEBERS Medical, we’re committed to making TMS more accessible to people around the world. That wraps up our conversation with Christian Hirschbeck, CEO of SEBERS Medical. His passion for advancing TMS technology is clear, and his vision for making TMS accessible, affordable, and effective is driving the next phase of growth for SEBERS Medical and the Blossom TMS device. Stay tuned for more updates as we continue to lead the way in TMS innovation!
TMS Coverage for Adolescents: What You Need to Know About Aetna’s Policy
Transcranial Magnetic Stimulation (TMS) is now available for adolescents as young as 15, and insurance providers like Aetna are expanding their coverage to meet this growing demand. As of now, Aetna has updated their policies to cover TMS for adolescents aged 15 and older with Major Depressive Disorder (MDD), but this shift is likely to inspire other insurance companies to follow suit. Key Points from Aetna’s TMS Coverage Policy: Are Other Insurance Providers Following? While Aetna is a leader in expanding adolescent TMS coverage, many other insurance providers are likely to follow this trend. Given the effectiveness and growing recognition of TMS as a non-invasive treatment for MDD, it’s expected that other insurers like Humana and BlueCross BlueShield may soon update their policies to include adolescent coverage as well. What Should Providers Do? For clinics and providers, the best practice is to check directly with insurance companies regarding their specific coverage for adolescent TMS. Since each insurance provider has its own set of guidelines, verifying coverage before initiating treatment is key to ensuring the best possible care for patients. Conclusion The expansion of TMS coverage for adolescents marks a significant step forward in treating mental health conditions in younger populations. As more insurance companies update their policies, TMS will become even more accessible, allowing more adolescents to benefit from this life-changing therapy. If you want to learn more about how Blossom TMS can help adolescents, visit our blog or contact us today. Source: https://www.aetna.com/cpb/medical/data/400_499/0469.html
Suicide Prevention Month: How TMS is Helping to Save Lives
September is Suicide Prevention Month in the U.S., a time to raise awareness about a crisis that affects millions of individuals and families. Suicide is the 10th leading cause of death in the country, with mental health challenges like depression playing a significant role in many cases. As a community, we must come together to spread the word about life-saving interventions like Transcranial Magnetic Stimulation (TMS), a non-invasive, effective treatment for depression. How TMS Can Help Address This Crisis TMS has emerged as a powerful tool in the fight against treatment-resistant depression, offering hope to individuals who haven’t found relief through traditional therapies like medication or talk therapy. By targeting specific areas of the brain linked to mood regulation, TMS can effectively reduce the symptoms of depression, including those that often lead to suicidal thoughts. In fact, clinical studies have demonstrated the positive impact of TMS in reducing depression and suicidal ideation. This non-invasive therapy is particularly beneficial for those who have not responded to antidepressants, providing a pathway to recovery that’s free from medication side effects. Why We Must Spread the Word TMS is part of the growing field of Interventional Psychiatry, which includes a range of innovative, non-drug treatments for mental health conditions. However, too few people are aware of these options. We need to amplify the conversation about the benefits of TMS, ensuring that both healthcare providers and patients know that help is available. By spreading the word, we can help our communities understand that there are effective treatments beyond medication. TMS, with its proven track record in treating depression, offers a ray of hope for those battling suicidal thoughts and feelings. Join the Effort At SEBERS Medical, we are committed to raising awareness about the benefits of TMS and other interventional psychiatry practices. Our Blossom TMS device is designed to make this life-saving treatment more accessible, with features that reduce overhead and improve clinic efficiency. As we recognize Suicide Prevention Month, let’s work together to ensure that those struggling with depression and suicidal ideation know that TMS can help. Together, we can make a difference in the fight against suicide. Learn More About TMSVisit our website to find out how TMS can help your clinic provide vital support to those in need. #SuicidePreventionMonth #TMS #InterventionalPsychiatry #MentalHealthAwareness #DepressionTreatment #BlossomTMS #SaveLives
Unlocking Profitability in TMS: Why Blossom TMS is a Smart Investment
Transcranial Magnetic Stimulation (TMS) has rapidly become one of the most effective treatments for depression and other mental health conditions. As its popularity grows, many clinic owners are asking themselves: how profitable is TMS, and what’s the best device to maximize that profit? The Growing Demand for TMS TMS is in high demand due to its efficacy in treating Major Depressive Disorder (MDD) without the side effects often associated with medications. Many clinics have turned to TMS as a reliable revenue stream, with a significant return on investment (ROI). Clinics performing TMS can charge between $225 and $300 per session, with treatment courses typically ranging from 30 to 36 sessions. This offers clinics a strong potential for profitability. However, maximizing profitability depends not only on demand but also on controlling costs—especially in terms of the device you choose. The Hidden Costs of Pay-Per-Use Models Some TMS devices on the market come with a pay-per-use model, meaning clinics must pay a fee for every treatment they provide. While this model might seem manageable at first, these fees can accumulate over time, significantly reducing profits. Let’s break it down: • Even a conservative estimate of 3 patients a month on average, that is over 600 sessions in a year. At a pay-per-use rate of $65 per session, this can amount to an additional$39,000 annually—on top of the device’s initial cost. • Pay-per-use models often require special caps or coils that need frequent replacement, increasing operational costs and further reducing profitability. Blossom TMS: Designed for Long-Term Savings The Blossom TMS device offers a clear advantage by eliminating the pay-per-use model entirely. With no costly disposables or session fees, clinic owners can retain more of their revenue. Here’s how Blossom TMS helps clinics save: * No Pay-Per-Use Fees: Unlike other models, Blossom TMS doesn’t charge clinics for each session, providing a predictable cost structure.* No Expensive Disposables: Blossom TMS is built for long-term use, with industry-leading coil cooling technology that reduces the need for frequent replacements.* Energy Efficiency: Blossom TMS runs on a standard 120V US outlet, reducing energy consumption and operational costs. Maximizing ROI with TMS With the right TMS device, clinic owners can achieve a strong ROI. Clinics offering TMS treatments can generate large earnings annually, depending on session pricing and patient volume. Without the burden of pay-per-use fees, these earnings translate more directly into profit. When comparing TMS devices, it’s important to consider not only the upfront cost but also long-term expenses tied to disposables, pay-per-use fees, and energy consumption. Blossom TMS stands out for its cost-effective design that supports clinics in providing quality care without hidden overhead costs. The Takeaway For clinics looking to expand into TMS, profitability is well within reach—especially when avoiding costly pay-per-use models. By choosing Blossom TMS, you’re investing in a future of predictable costs, enhanced treatment options, and long-term profitability.
TMS: First-Line Treatment for Depression?
The landscape of mental health treatment is rapidly evolving, and Transcranial Magnetic Stimulation (TMS) is at the forefront of this transformation. Traditionally used as a secondary or last-resort treatment for individuals who did not respond to antidepressant medications, TMS is now being considered a first-line treatment option for depression by many psychiatrists and clinics. The shift towards TMS is driven by its growing body of clinical evidence, superior safety profile, and potential for long-term relief. The Case for TMS as a First-Line Treatment For decades, antidepressant medications have been the primary treatment for major depressive disorder (MDD). However, not all patients respond positively to these medications, and many experience adverse side effects such as weight gain, fatigue, and sexual dysfunction. Moreover, medications often need to be taken over a long period, and in some cases, patients must try multiple drugs before finding one that works, if they find relief at all. TMS offers an alternative. It is a non-invasive, drug-free treatment that uses magnetic pulses to stimulate areas of the brain involved in mood regulation. Multiple studies have demonstrated that TMS can achieve higher remission rates in patients with depression, with significantly fewer side effects compared to antidepressants. A large-scale clinical trial showed that TMS was more effective than additional antidepressants for treatment-resistant patients, and the success of TMS in this challenging population is contributing to its growing acceptance as a primary treatment option. Long-Term Relief with Minimal Side Effects A key reason behind the increased adoption of TMS is the long-term relief it offers. A typical TMS treatment protocol involves daily sessions over several weeks, and patients who respond positively often maintain their improvements for months or even years. Studies have shown that 68% of patients who benefit from TMS continue to experience positive outcomes for at least 12 months, reducing the need for ongoing treatments or medications. Moreover, TMS has a low side-effect profile. The most common side effects include mild scalp discomfort or headaches, which generally subside after the first few sessions. This contrasts with the more severe and persistent side effects often associated with antidepressant medications, making TMS an appealing option for those who prioritize quality of life and minimizing treatment-related discomfort. The Future of TMS As TMS continues to gain recognition, its potential to revolutionize depression treatment is becoming clearer. Advancements in TMS technology, including the development of more precise stimulation techniques and individualized treatment protocols, are improving its efficacy and accessibility. Additionally, insurance companies are expanding coverage for TMS, which is further removing barriers for patients seeking this cutting-edge therapy. With more clinics offering TMS and its success rate continuing to rise, it’s no surprise that psychiatrists are considering it as a first-line treatment for depression. The non-invasive nature, minimal side effects, and long-lasting relief make TMS a valuable tool in the fight against depression, offering hope for individuals who may have previously found their options limited. TMS is reshaping the future of depression treatment. As a first-line treatment, it holds significant promise for individuals suffering from MDD who are seeking effective, non-drug alternatives to traditional therapies. With more research supporting its efficacy and accessibility on the rise, TMS is poised to become a mainstay in the treatment of depression. Sources: